Understanding PPO Insurance for Addiction Treatment
PPO insurance rehab offers flexibility and choice when seeking addiction treatment. Here’s what you need to know:
- What it is: A Preferred Provider Organization (PPO) is a health insurance plan that gives you access to a network of providers while still covering out-of-network care
- No referrals needed: You can see specialists and enter rehab programs without getting permission from a primary care physician
- Coverage included: Medical detox, inpatient treatment, outpatient programs, therapy, and Medication-Assisted Treatment (MAT)
- Cost factors: You’ll pay deductibles, copays, and coinsurance—with lower costs for in-network facilities
- Out-of-network option: PPO plans typically cover 50-60% of out-of-network rehab costs, giving you more treatment choices than HMO or EPO plans
If you’re struggling with addiction, you’re not alone. Approximately 17% of the U.S. population struggles with some form of drug or alcohol addiction, yet 94% of people with substance use disorders don’t receive treatment. The biggest barrier? Understanding insurance coverage.
PPO plans offer significant advantages for addiction treatment. Unlike restrictive HMO plans, PPOs let you choose from a wider range of rehab facilities—both in your network and outside it. You won’t need a referral to start treatment, which means faster access to care when you need it most. However, coverage details vary widely by plan, and navigating deductibles, pre-authorization requirements, and medical necessity criteria can feel overwhelming when you’re already at your lowest point.
Understanding your PPO benefits before you start treatment helps you avoid surprise bills and find the right level of care. Whether you need medical detox, residential treatment, or outpatient support, knowing what your plan covers—and what you’ll pay out of pocket—makes it easier to focus on what matters most: your recovery.
At Pine Meadows Recovery in Kenosha, Wisconsin, we work with most major PPO insurance plans and help clients navigate the verification process to understand their coverage for addiction treatment. Our team has extensive experience helping individuals maximize their PPO insurance rehab benefits while accessing evidence-based, compassionate care tailored to their unique needs.
PPO insurance rehab vocab to learn:
- Does insurance cover drug rehabilitation
- Does insurance cover rehab
- Does private health insurance cover rehab
Understanding PPO Insurance Rehab and How It Works
A Preferred Provider Organization (PPO) is a type of managed care plan designed to give members the most freedom possible when selecting healthcare providers. In addiction recovery, this freedom is a game-changer. Unlike other plans that tether you to a very specific list of doctors, a PPO allows you to seek care from almost any licensed facility.
The “Preferred” part of the name refers to the insurance company’s network of “in-network” providers. These are facilities and doctors who have agreed to provide services at a pre-negotiated, discounted rate. When you use an in-network PPO insurance rehab, your out-of-pocket costs are significantly lower. However, the standout feature of a PPO is that it still provides coverage if you choose an “out-of-network” provider. You will likely pay more in the form of higher coinsurance or a separate deductible, but the insurance company will still foot a portion of the bill.
One of the most vital aspects of a PPO for someone in crisis is the lack of a Primary Care Physician (PCP) referral requirement. In many other health plans, you must first see your family doctor, explain your situation, and wait for them to write a formal referral before the insurance company will pay for a specialist or a rehab program. With a PPO, you can bypass this step entirely. If you realize today that you need help, you can call a treatment center like Pine Meadows Recovery directly. This removes a significant administrative barrier and can save precious time when someone is ready to accept help. For a deeper dive into these mechanics, you can read more about unpacking your insurance coverage.
Types of Addiction Services Covered by PPO Insurance Rehab
Because of the Affordable Care Act (ACA), most PPO plans are required to cover essential health benefits, which include mental health and substance use disorder services. While every specific policy is different, a standard PPO insurance rehab plan typically covers several levels of care:
- Medical Detox: This is often the first step in recovery. It involves 24/7 medical supervision to manage withdrawal symptoms safely. Because detox is often considered a medical emergency or necessity, it is widely covered by PPO plans.
- Inpatient/Residential Treatment: This involves staying at a facility for a set period, typically between 30 and 105 days. PPOs are often favored here because they may cover residential programs that offer more personalized or holistic environments.
- Outpatient Programs (OP/IOP/PHP): These programs allow you to receive intensive therapy during the day while returning home at night. The typical stay for outpatient programs usually runs up to 120 days.
- Medication-Assisted Treatment (MAT): PPOs generally cover the medications used to treat opioid and alcohol use disorders, such as buprenorphine, naltrexone, or methadone, alongside behavioral therapy.
- Dual Diagnosis Treatment: Many people struggling with addiction also face co-occurring mental health issues like depression or PTSD. PPO plans are required to cover treatment for these “dual” conditions under parity laws.
Comparing PPO to HMO, EPO, and POS Plans
Choosing the right plan often feels like trying to solve a puzzle. When looking at PPO insurance rehab options, it helps to see how they stack up against other common models:
| Feature | PPO (Preferred Provider) | HMO (Health Maintenance) | EPO (Exclusive Provider) | POS (Point of Service) |
|---|---|---|---|---|
| Out-of-Network Coverage | Yes (Higher cost) | No (Except emergencies) | No | Yes (With referral) |
| Referral Needed? | No | Yes | No | Yes |
| PCP Required? | No | Yes | No | Yes |
| Monthly Premium | Generally Higher | Generally Lower | Moderate | Moderate |
| Autonomy Level | Very High | Low | Moderate | Moderate |
HMOs are often the most restrictive; if you go to a rehab center outside their small network, they may pay $0. EPOs are a middle ground—they don’t require referrals, but like HMOs, they usually offer zero coverage for out-of-network care. POS plans are a hybrid that allows out-of-network care but requires you to jump through the hoop of getting a PCP referral first. For those seeking the highest level of autonomy and the widest choice of facilities, the PPO remains the gold standard.
Key Benefits of Using PPO Insurance for Rehab
The primary benefit of PPO insurance rehab is access. When you are looking for a life-saving service, you don’t want to be told that the only available facility is 200 miles away or has a six-month waiting list. Because PPOs have such large networks and offer out-of-network benefits, your “menu” of treatment options is much larger.
This flexibility allows you to seek out specialized care. Perhaps you need a program that focuses on trauma-informed therapy, or maybe you are looking for a facility that offers private health insurance for rehab perks like equine therapy or holistic wellness. Many high-end or “luxury” facilities accept PPO insurance because the reimbursement rates and out-of-network flexibility align with their clinical models.
Furthermore, PPO plans often allow for out-of-state treatment. While Pine Meadows Recovery serves the Kenosha, Wisconsin area, we understand that some individuals find success by removing themselves from their local environment. A PPO plan makes this transition much easier. By choosing a plan with high clinical excellence and personalized care, you are investing in a higher success rate. Statistics suggest that inpatient treatment tends to have a higher success rate because it allows you to completely focus on yourself and your recovery without local distractions.
Navigating Costs: Deductibles, Copays, and Out-of-Network Care
While PPOs offer the most freedom, they aren’t “free.” Understanding the financial terminology is crucial for planning your stay.
- Deductibles: This is the amount you pay out of pocket before your insurance starts to chip in. If you have a $3,000 deductible, you must pay that amount toward your care first. Many people find they have already met part of their deductible through other medical visits earlier in the year.
- Copayments (Copays): These are fixed fees you pay for specific services, such as $50 for an outpatient therapy session.
- Coinsurance: This is your share of the costs of a covered service, calculated as a percentage. For example, if your plan’s allowed amount for an inpatient stay is $10,000 and you’ve met your deductible, your 20% coinsurance would be $2,000. The insurance pays the remaining 80%.
- Out-of-Pocket Maximum: This is the most you will have to pay for covered services in a plan year. Once you reach this limit, the insurance company pays 100% of the allowed amount.
When using PPO insurance rehab for an out-of-network facility, the cost-sharing is usually higher. For instance, while an in-network facility might have a 20% coinsurance, an out-of-network one might have 50%. It is also important to note that grandfathered health plans—those created before March 23, 2010—may not be required to follow all ACA rules, which could impact your total costs. Always check your Summary of Benefits and Coverage (SBC) to see your specific reimbursement rates.
How to Verify Your PPO Insurance Rehab Benefits
Verifying your benefits is the most important step before checking into a facility. You don’t want to be halfway through detox only to find out your plan doesn’t cover that specific level of care.
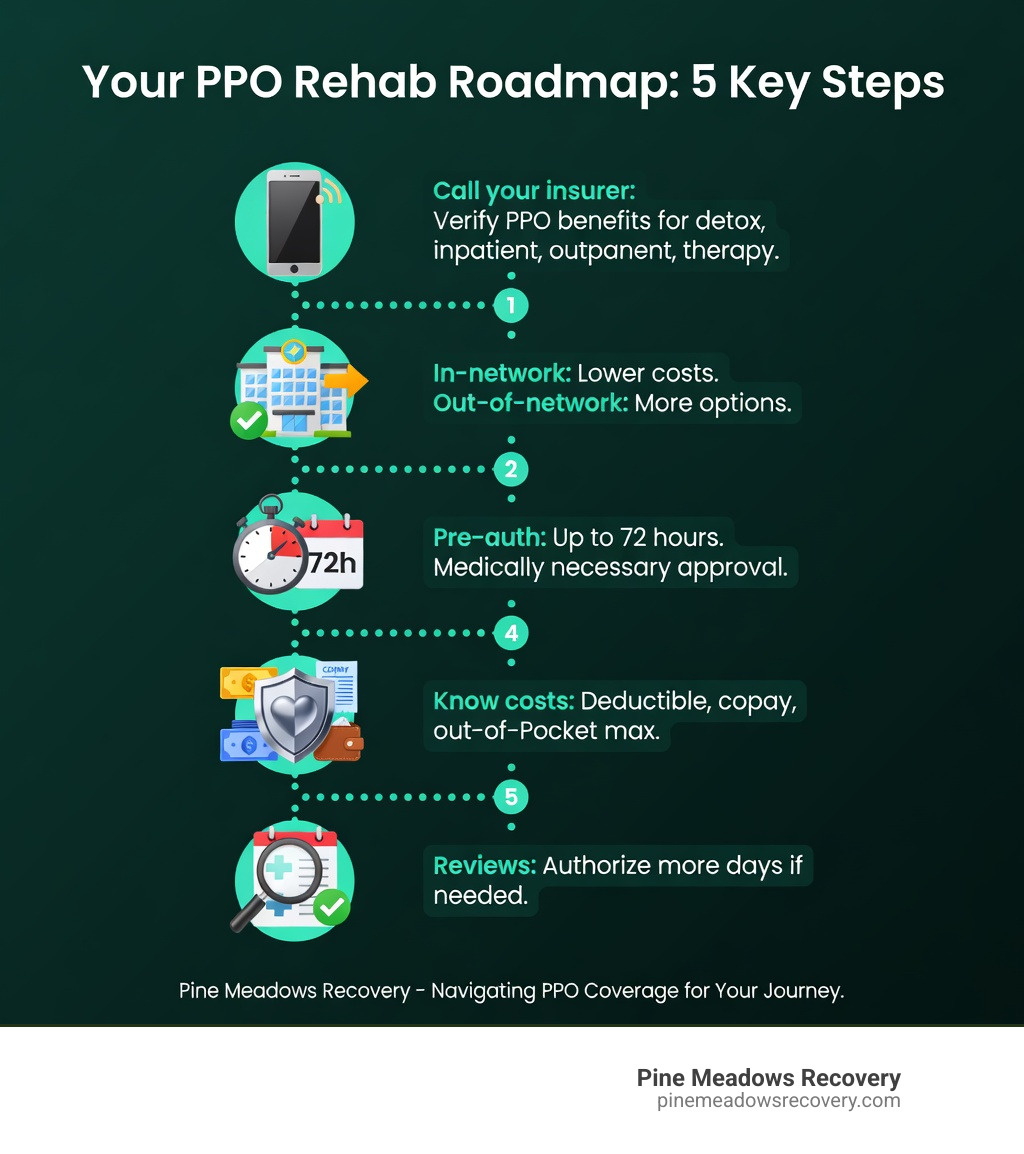
To start, call the “Member Services” number on the back of your insurance card. Have your policy ID ready and ask specific questions:
- Does my plan cover residential addiction treatment?
- What is my remaining deductible for the year?
- Is “medical necessity” required for inpatient care?
- Do I need pre-authorization?
Most insurance providers can take up to 72 hours to notify a center that care has been authorized. This is a critical window. If you need immediate admission, some facilities allow you to pay an out-of-pocket deposit while waiting for the 72-hour authorization window to close, though this carries a risk if the claim is eventually denied. To make this easier, we offer a dedicated insurance verification tool to help you get answers quickly.
Finding the Right PPO Insurance Rehab Center
Once you know what your insurance will pay for, you need to find a facility that matches your clinical needs. Don’t just pick the first name in an in-network directory. Look for:
- Facility Reputation: Check reviews and clinical credentials.
- Evidence-Based Programs: Ensure they use proven methods like Cognitive Behavioral Therapy (CBT).
- Telehealth Options: Wisconsin has many facilities offering telehealth, which can be great for aftercare.
- Specialized Tracks: Does the facility handle co-occurring disorders?
At Pine Meadows Recovery, we focus on a client-centered approach. We believe that finding the right fit is about more than just a list of covered services; it’s about finding a place where you feel safe and supported. You can read more here about how to find out if your insurance covers rehab.
Legal Protections and Overcoming Claim Denials
It is a common fear: “What if they say no?” Fortunately, federal laws provide significant protections. The Mental Health Parity and Addiction Equity Act (MHPAEA) requires that insurance companies treat mental health and substance use disorder benefits the same way they treat medical and surgical benefits. They cannot, for example, set a $5,000 limit on rehab if they don’t have a similar limit on heart surgery.
If your PPO insurance rehab claim is denied, do not panic. Common reasons for denial include a perceived lack of “medical necessity” or administrative errors in the paperwork. You have the right to:
- Request a Reason: The insurer must provide a written explanation.
- Appeal: You can file an internal appeal asking the company to reconsider.
- External Review: If the internal appeal fails, you can often request an independent third party to review the case.
If insurance coverage is insufficient, there are alternative payment options. Many facilities offer sliding scale fees based on income, payment plans, or even scholarships. Some people also utilize SAMHSA grants or personal loans to bridge the gap.
Frequently Asked Questions about PPO Rehab
Do I need a doctor’s referral to start rehab with a PPO?
No. One of the biggest advantages of a PPO plan is that you do not need a referral from a primary care physician to access addiction treatment or see a specialist. You can contact a treatment facility directly to begin the admissions process.
Does PPO insurance cover out-of-state addiction treatment?
Generally, yes. Most PPO plans provide coverage for providers across the country, though they may distinguish between in-network and out-of-network costs. If the out-of-state facility is “in-network” for your specific PPO provider (like Blue Cross Blue Shield), your costs may remain low even if you cross state lines.
What happens if my PPO insurance claim for rehab is denied?
If a claim is denied, you should first review the Explanation of Benefits (EOB) to understand why. You can work with the rehab facility’s billing department to file an appeal. Many denials are overturned upon providing additional clinical documentation that proves the “medical necessity” of the treatment.
Conclusion
Navigating PPO insurance rehab can feel like learning a second language, but it is a journey worth taking. With the flexibility of a PPO, you have the power to choose a facility that offers the evidence-based, holistic care you deserve. Whether you are dealing with a long-term struggle or a recent crisis, understanding your benefits is the first step toward reclaiming your life.
At Pine Meadows Recovery in Kenosha, Wisconsin, we are dedicated to providing client-centered care that focuses on long-term healing. We know that the administrative side of recovery is the last thing you want to deal with, which is why our team is here to help you decode your policy and maximize your benefits.
Don’t let insurance confusion stand in the way of your health. Verify your PPO insurance for rehab today and take the first step toward a brighter, sober future.
