Understanding Your Path to Affordable Recovery
Does insurance cover drug rehabilitation? Yes, in most cases health insurance does cover drug rehabilitation services. Thanks to the Affordable Care Act and the Mental Health Parity and Addiction Equity Act, most insurance plans must provide coverage for substance use disorder treatment as an essential health benefit. Coverage typically includes:
- Medical detoxification – Supervised withdrawal management
- Inpatient/residential treatment – 24-hour care and housing
- Outpatient programs – Flexible treatment while living at home
- Medication-assisted treatment (MAT) – Medications to support recovery
- Therapy and counseling – Individual and group sessions
- Aftercare programs – Ongoing support post-treatment
The specific amount covered depends on your individual plan, with most insurance paying between 60-90% of treatment costs after deductibles are met.
Financial concerns are often the single biggest reason people delay seeking help. In 2021, over 46 million Americans aged 12 or older suffered from a substance use disorder, yet 94% did not receive treatment. However, addiction is far more expensive than treatment. The cost of addiction to the United States exceeds $532 billion annually due to lost income and health issues. Even a $10-a-day habit costs over $30,000 in a decade—more than many treatment programs.
At Pine Meadows Recovery in Kenosha, Wisconsin, we help individuals verify benefits and work with insurance providers to maximize coverage. We understand that does insurance cover drug rehabilitation is often your first question, and we’re here to provide clear answers.
Quick does insurance cover drug rehabilitation terms:
Does Insurance Cover Drug Rehabilitation?
For most Americans, health insurance does cover drug rehabilitation. Significant legislative changes have transformed how insurance companies approach addiction treatment.
The Affordable Care Act (ACA) designated substance use disorder services as an “Essential Health Benefit.” This means Marketplace plans, Medicaid expansion, and most small group plans are legally required to cover addiction treatment as a medical condition. You can learn more at HealthCare.gov.
The Mental Health Parity and Addiction Equity Act (MHPAEA) requires most group health plans to provide substance use benefits that are no more restrictive than medical and surgical benefits. You shouldn’t face higher deductibles or stricter limits for addiction care compared to physical health services. Together, these laws ensure financial barriers are lessened for those seeking help in Kenosha, Wisconsin. Read our guide: Yes, Your Insurance Likely Covers Rehab: Here’s How to Find Out.
How Much Does Drug Rehabilitation Cost With Insurance?
Insurance rarely covers 100% of the cost. Your out-of-pocket expenses depend on:
- Deductible: The amount you pay before insurance starts contributing.
- Copayment (Copay): A fixed amount you pay for a covered service.
- Coinsurance: Your share of the cost, calculated as a percentage.
- Out-of-Pocket Maximum: The most you have to pay for covered services in a plan year.
Marketplace plans are tiered: Bronze plans have lower premiums but higher out-of-pocket costs (covering ~60%), while Platinum plans have the highest premiums but lowest out-of-pocket costs (covering ~90%).
| Feature | HMO | PPO |
|---|---|---|
| Premiums | Generally lower | Generally higher |
| Deductibles | Low to moderate | Moderate to high |
| Copay/Coinsurance | Fixed copays, lower in-network | Higher, especially out-of-network |
| Out-of-Pocket Max | Typically lower | Higher for out-of-network |
| Referrals | Required for specialists | Not required |
| Provider Choice | Limited to network | Flexible; out-of-network allowed |
Does Insurance Cover Drug Rehabilitation for Pre-existing Conditions?
The ACA prohibits insurance companies from denying coverage or charging more based on pre-existing conditions, including addiction. Addiction is recognized as a chronic medical condition, much like diabetes. This ensures that your past health history cannot be used to deny you the coverage you need for rehabilitation. Find more information via Medical News Today.
Understanding Different Insurance Plans and Their Benefits
Navigating the alphabet soup of insurance plans can feel like cracking a secret code. But understanding the basics of HMOs, PPOs, and POS plans can help you maximize your benefits for addiction treatment.
-
HMO (Health Maintenance Organization): These plans typically have lower monthly premiums but offer less flexibility. You usually need to choose a primary care physician (PCP) within the plan’s network, and that PCP must refer you to any specialists, including behavioral health providers. If you go out-of-network, the services generally won’t be covered, except in emergencies. For addiction treatment, this means ensuring your chosen facility and all its providers are part of your HMO’s network and securing a referral from your PCP.
-
PPO (Preferred Provider Organization): PPO plans offer more flexibility than HMOs. You typically don’t need a PCP or a referral to see a specialist. You can see out-of-network providers, but you’ll pay a higher cost (higher copayments, coinsurance, and deductibles). This flexibility can be valuable if you have a specific treatment center in mind that might be out-of-network, though it will come with a higher financial burden.
-
POS (Point of Service): POS plans combine features of both HMOs and PPOs. You often choose a PCP within the network, who can then refer you to in-network specialists (like an HMO). However, you also have the option to go out-of-network for care, similar to a PPO, but at a higher cost.
For us at Pine Meadows Recovery, we work with a wide range of insurance providers that offer these different types of plans. We understand that maximizing your in-network benefits is key to affordable treatment. When you consider treatment, check if our facility and our clinicians are considered “in-network” with your specific plan. This typically results in lower out-of-pocket costs for you.
To gain a deeper understanding of how these different plans impact your coverage for rehabilitation services, we recommend exploring our comprehensive guide: Decoding Your Policy: What Private Health Insurance Really Covers for Rehab.
Types of Addiction Treatment Services Covered
Insurance typically covers a comprehensive range of evidence-based addiction treatment services, recognizing that effective recovery often requires a multi-faceted approach. These services are designed to address the physical, psychological, and social aspects of substance use disorder.
Here are the types of services generally covered:
-
Medical Detoxification: This is often the first step in treatment, especially for substances that cause severe physical withdrawal symptoms. Medical detox provides a safe, supervised environment where medical professionals manage withdrawal symptoms with medications and supportive care. Insurance typically covers this crucial phase, as it’s a medical necessity to stabilize a patient before further treatment.
-
Inpatient/Residential Treatment: These programs involve living at a treatment facility for an extended period (often 30, 60, or 90 days). They provide 24-hour care, structured therapy, and a supportive environment away from triggers. Inpatient rehab is generally the most intensive and, consequently, the most expensive level of care, but it’s often covered by insurance when deemed medically necessary.
-
Outpatient Programs: For individuals who don’t require 24/7 supervision or who have completed inpatient care, outpatient programs offer flexibility. These include:
- Partial Hospitalization Programs (PHP): Often called “day treatment,” PHPs involve several hours of therapy and medical monitoring per day, several days a week, while the client returns home in the evenings.
- Intensive Outpatient Programs (IOP): IOPs offer fewer hours per week than PHPs, allowing clients to maintain work, school, or family commitments.
Both PHPs and IOPs include individual and group therapy, life skills training, and relapse prevention education. Insurance typically covers these programs.
-
Medication-Assisted Treatment (MAT): This approach combines medications (like buprenorphine, naltrexone, or acamprosate) with counseling and behavioral therapies. MAT is highly effective for treating opioid and alcohol use disorders and is increasingly covered by insurance as an evidence-based practice. Medicare Part D may also cover medically necessary medications for alcohol addiction treatment.
-
Evidence-Based Therapy: The core of addiction treatment involves various therapeutic modalities proven to be effective. These include:
- Cognitive Behavioral Therapy (CBT): Helps clients identify and change unhealthy thought patterns and behaviors.
- Dialectical Behavior Therapy (DBT): Focuses on emotional regulation, mindfulness, and interpersonal effectiveness.
- Group Therapy: Provides peer support and shared experiences.
- Family Counseling: Addresses family dynamics that may contribute to or be affected by addiction.
These therapeutic interventions are widely covered by insurance.
-
Aftercare Programs: Recovery is a lifelong journey, and aftercare is crucial for sustained sobriety. This can include ongoing therapy, support groups, and alumni programs. Insurance coverage for aftercare varies, but many plans cover continued outpatient therapy.
At Pine Meadows Recovery, we offer a full spectrum of these evidence-based services, custom to your individual needs. We believe in personalized programs and holistic healing to support your journey to long-term recovery.
Public Insurance Options: Medicare and Medicaid
For many individuals, public insurance programs like Medicare and Medicaid provide essential coverage for addiction treatment. These programs are vital safety nets for specific populations across the country, including in Wisconsin.
Medicare is a federal health insurance program primarily for people aged 65 or older, some younger people with disabilities, and people with End-Stage Renal Disease. Medicare coverage for addiction treatment typically includes:
- Medicare Part A (Hospital Insurance): Covers inpatient hospital stays, including services received during an inpatient drug or alcohol rehabilitation program. This includes room and board, nursing care, and other hospital services.
- Medicare Part B (Medical Insurance): Covers outpatient services, such as doctor visits, mental health services (including individual and group therapy), partial hospitalization programs, and other outpatient addiction treatment. It also covers medically necessary diagnostic tests.
- Medicare Part D (Prescription Drug Coverage): May cover medications used in addiction treatment, such as those for Medication-Assisted Treatment (MAT), if they are medically necessary.
Medicaid is a joint federal and state program that provides health coverage to millions of Americans, including low-income adults, children, pregnant women, elderly adults, and people with disabilities. In states like Wisconsin that have expanded Medicaid under the ACA, more low-income individuals qualify. Medicaid is a critical source of funding for addiction treatment, and it’s particularly important given the statistics: nearly 12% of adults who are recipients of Medicaid have a substance use disorder.
Medicaid typically covers a broad range of addiction treatment services, including:
- Inpatient and outpatient rehabilitation
- Detoxification
- Medication-Assisted Treatment (MAT)
- Counseling and therapy
- Case management
In most states, Medicaid recipients do not pay a copay for these services. However, it’s important to note that not all treatment facilities accept Medicaid, so verifying with the facility beforehand is crucial.
If you’re exploring public insurance options or other forms of assistance, our guide, An Essential Guide to Finding Addiction Help, can provide more valuable information. We are committed to helping you find the resources you need to get treatment.
How to Verify Your Coverage and Start Treatment
Understanding that does insurance cover drug rehabilitation is just the first step. The next is to actively verify your specific benefits and steer the admissions process. While it might seem daunting, we’re here to help simplify it for you.
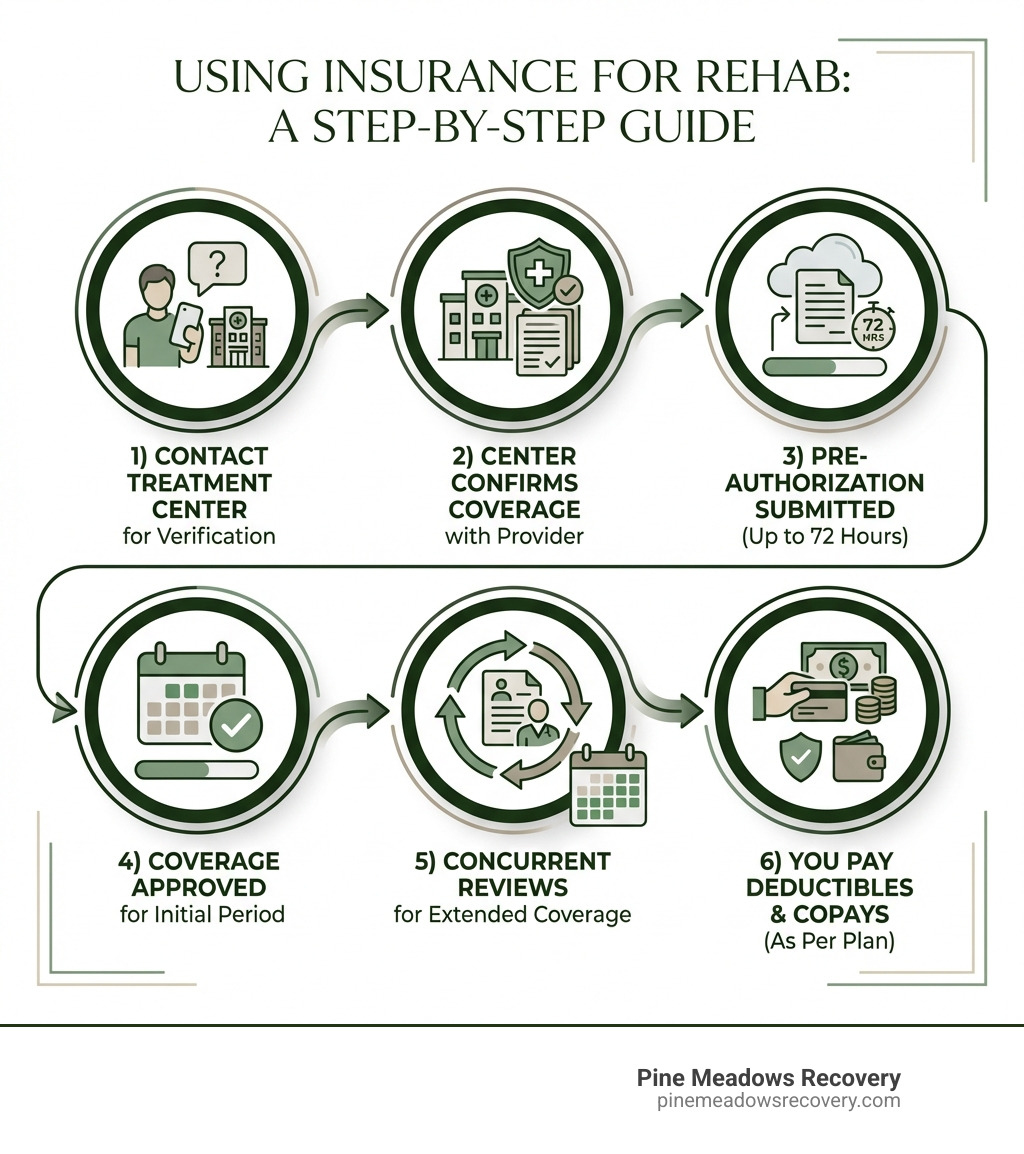
Here’s how the process typically works at Pine Meadows Recovery:
-
Initial Contact and Information Gathering: When you reach out to us, our admissions team will gather some basic information about your insurance provider and policy details. This usually includes your insurance company name, policy number, and date of birth.
-
Insurance Verification: We then contact your health insurance provider directly on your behalf to confirm your coverage and benefits. This involves understanding your deductible, copayments, coinsurance, out-of-pocket maximum, and what specific addiction treatment services are covered under your plan. We also check if we are an in-network provider for your plan, which can significantly reduce your costs.
-
Pre-Authorization: Many insurance companies require “pre-authorization” or “pre-certification” for addiction treatment services, especially for inpatient or residential care. This means the insurance company needs to approve the treatment plan before you begin. Our team will submit the necessary clinical information to your insurance provider to secure this authorization. Be aware that insurance providers can take up to 72 hours to notify about authorization.
-
Clinical Necessity and Concurrent Reviews: Insurance companies base their authorization on “medical necessity” and “clinical necessity.” Our clinical team will provide your insurance company with detailed information about your condition and the recommended level of care. Authorization is often granted in short increments (e.g., a few days or a week at a time). To continue coverage, we conduct “concurrent reviews,” providing regular updates on your clinical progress and ongoing medical necessity. This ensures your treatment aligns with your plan’s requirements.
-
Understanding Your Financial Responsibility: Once your benefits are verified and pre-authorization is obtained (if required), we’ll clearly explain your financial responsibility. This includes any deductibles you need to meet, copayments for services, or coinsurance percentages. We believe in transparency so there are no surprises.
What if you want to start treatment immediately, but authorization is still pending? In such cases, you might have the option to pay a deposit out-of-pocket to begin treatment. However, it’s important to understand that doing so carries the risk of denial of insurance coverage if authorization is not ultimately granted. We always advise waiting for authorization when possible to avoid unexpected costs.
Our goal at Pine Meadows Recovery is to make this process as smooth as possible so you can focus on what truly matters: your recovery. We are experts in navigating insurance complexities for our clients in Kenosha, Wisconsin. For a more detailed look at this process, visit our Insurance Verification page.
Frequently Asked Questions about Rehab Coverage
What if I don’t have insurance?
Don’t let a lack of insurance deter you. Options include:
- State-Funded Rehab: Wisconsin offers programs for eligible individuals based on income.
- SAMHSA Grants: Federal block grants help fund services for those who lack access.
- Payment Plans: Many centers, including ours, offer sliding scale fees or flexible payment plans.
- Employer Assistance (EAPs): Workplace programs can provide confidential counseling and referrals.
- Non-Profits: Organizations like the Salvation Army offer low-cost or free programs.
Reach out to discuss your situation. SAMHSA offers a guide on How to Pay for Mental Health, Drug, or Alcohol Treatment.
Can insurance limits affect the length of my treatment?
Yes. Insurance companies determine coverage duration based on “medical necessity.” Our clinical team provides regular updates to justify continued care. While programs often run in 30, 60, or 90-day increments, authorization is typically granted in shorter blocks. We work closely with providers to advocate for the length of treatment necessary for sustainable recovery.
Are holistic or luxury amenities covered by insurance?
Insurance covers evidence-based medical and therapeutic treatments deemed medically necessary, such as detox, counseling, and MAT. However, luxury amenities—like gourmet meals, spa treatments, or private rooms—are usually not covered and must be paid out-of-pocket. At Pine Meadows Recovery, we prioritize clinical effectiveness and holistic care that promotes healing. Learn more about What We Treat.
Conclusion
Understanding whether does insurance cover drug rehabilitation is a crucial first step on your path to recovery. Thanks to federal mandates like the Affordable Care Act and the Mental Health Parity and Addiction Equity Act, most health insurance plans are now required to cover addiction treatment as an essential health benefit, treating it with the same importance as any other medical condition. This means that financial barriers to treatment are significantly lower than they once were.
While your specific out-of-pocket costs will depend on your individual plan’s deductibles, copayments, and coinsurance, rest assured that options exist. Whether you have private insurance, Medicare, Medicaid, or no insurance at all, there are pathways to accessing the care you need.
At Pine Meadows Recovery in Kenosha, Wisconsin, we are dedicated to providing personalized programs, holistic healing, and evidence-based care to help you achieve long-term recovery. We understand the complexities of insurance coverage and are here to guide you through the verification process, advocating for your right to comprehensive treatment. Don’t let uncertainty about insurance keep you from taking the most important step towards a healthier, happier life.
Your recovery journey can begin today. We invite you to reach out to us for a confidential conversation.
